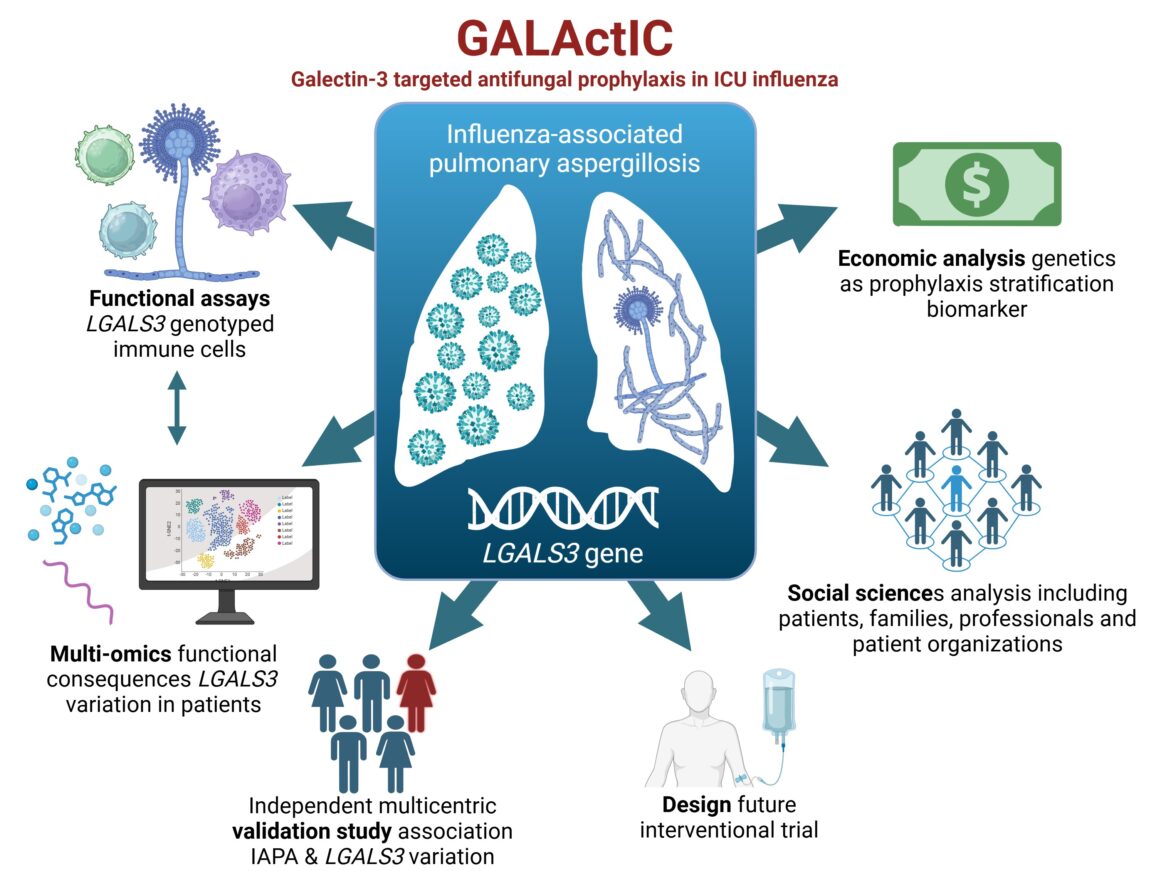
Influenza-associated pulmonary aspergillosis (IAPA) occurs as a complication in up to 20% of critically ill influenza patients and is associated with a mortality rate of 50%, twice as high as in influenza-only patients. Diagnosing IAPA is difficult, resulting in delayed initiation of antifungal therapy and increased mortality. Hence, rapid identification of patients at risk for IAPA is urgently needed to allow patient stratification for personalized antifungal prophylaxis. We have recently identified a genetic variant in LGALS3, associated with the development of IAPA. LGALS3 encodes galectin-3, which is implicated in antifungal immunity. In a discovery cohort, more than 65% of variant carriers developed IAPA. Here, we aim to validate the functional and clinical value of LGALS3 genetics for patient stratification in targeted antifungal prophylaxis. Functional assays using LGALS3 genotyped immune cells will be used to assess their phagocytosis and Aspergillus killing potential. These data will be integrated with immune/omics marker datasets to better understand the functional consequences of LGALS3 variation. The association between the LGALS3 variation and IAPA will be further validated in a large independent multicentric international cohort. We will also design and prepare a future interventional trial protocol using LGALS3 variation as a companion biomarker for patient stratification in personalized antifungal prophylaxis. Health economic analyses on the use of genetics as biomarker for stratifying prophylaxis will be performed, as well as a social sciences analyses with input of patients and their families, healthcare professionals and patient organizations to ensure efficient implementation of genetics-driven prophylaxis in an ICU context.

